Types of Gangrene
There are three different types of gangrene that affect the body in different ways. These three types are commonly known as Wet Gangrene, Dry Gangrene and Gas Gangrene. You can find out in depth about each form of this disease below.
Wet Gangrene
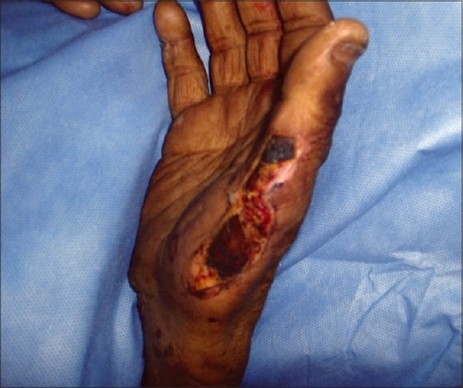
Wet Gangrene occurs in naturally moist tissue and organs such as the mouth, bowel, lungs, cervix and vulva. Bedsores occurring on body parts such as the sacrum, buttocks and heels- although not usually moist areas- are categorized as wet gangrene infections. It is characterized by numerous bacteria and has a poor prognosis compared to dry gangrene due to septicemia. In wet gangrene, the tissue is infected by saprogenic micro organisms which cause tissue to swell and emit a fetid smell. Wet gangrene usually develops rapidly due to blockage of arterial blood flow. The affected part is saturated with stagnant blood, which promotes the rapid growth of bacteria. The toxic products formed by bacteria are absorbed, causing systemic manifestation of septicimia and finally death. The affected part is edematous, soft, putrid, rotten and dark. The darkness in wet gangrene occurs due to the same mechanism as in dry gangrene. Wet gangrene is coagulative necrosis progressing to liquefactive neurosis.
Dry Gangrene
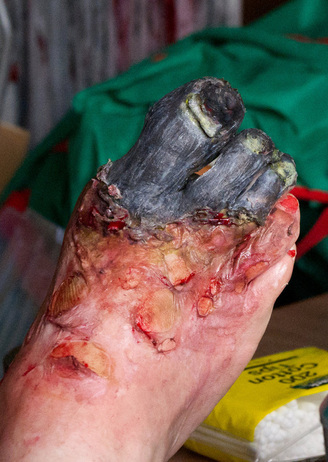
Dry gangrene begins at the distal part of the limb due to ischemia, and often occurs in the toes and feet of elderly patients due to arteriosclerosis and thus, is also known as senile gangrene. Dry gangrene is mainly due to arterial occlusion. There is limited putrefaction and bacteria fail to survive. Dry gangrene spreads slowly until it reaches the point where the blood supply is adequate to keep tissue viable. The affected part is dry, shrunken and dark reddish-black, resembling mummified flesh. The dark coloration is due to liberation of heoglobin from hemolyzed red blood cells, which is acted upon by hydrogen sulfide (H2S) produced by the bacteria, resulting in formation of black iron sulfide that remains in the tissues.The line of separation usually brings about complete separation, with eventual falling off of the gangrenous tissue if it is not removed surgically, also called autoamputation.
Dry gangrene is actually a form of coagulative necrosis. If the blood flow is interrupted for a reason other than severe bacterial infection, the result is a case of dry gangrene. People with impaired peripheral blood flow, such as diabetics, are at greater risk of developing dry gangrene.
The early signs of dry gangrene are a dull ache and sensation of coldness in the affected area along with pallor of the flesh. If caught early, the process can sometimes be reversed by vascular surgery. However, if necrosis sets in, the affected tissue must be removed just as with wet gangrene.
Dry gangrene is actually a form of coagulative necrosis. If the blood flow is interrupted for a reason other than severe bacterial infection, the result is a case of dry gangrene. People with impaired peripheral blood flow, such as diabetics, are at greater risk of developing dry gangrene.
The early signs of dry gangrene are a dull ache and sensation of coldness in the affected area along with pallor of the flesh. If caught early, the process can sometimes be reversed by vascular surgery. However, if necrosis sets in, the affected tissue must be removed just as with wet gangrene.
Gas Gangrene
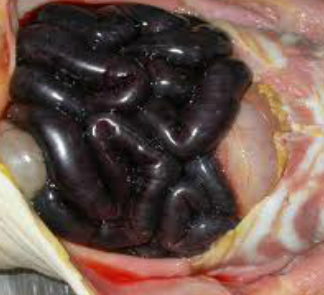
Gas gangrene is a bacterial infection that produces gas within tissues. It is a deadly form of gangrene usually caused by Clostridium perfringens bacteria. Infection spreads rapidly as the gases produced by bacteria expand and infiltrate healthy tissue in the vicinity. Because of its ability to quickly spread to surrounding tissues, gas gangrene should be treated as a medical emergency.
Gas gangrene is caused by a bacterial exotoxin-producing clostridial species, which are mostly found in soil and other anaerobes (e.g., Bacteroides and anaerobic streptococci). These environmental bacteria may enter the muscle through a wound and subsequently proliferate in necrotic tissue and secrete powerful toxins. These toxins destroy nearby tissue, generating gas at the same time. A gas composition of 5.9% hydrogen, 3.4% carbon dioxide, 74.5% nitrogen, and 16.1% oxygen was reported in one clinical case.
Gas gangrene can cause necrosis, gas production, and sepsis. Progression to toxemia and shock is often very rapid.
Gas gangrene is caused by a bacterial exotoxin-producing clostridial species, which are mostly found in soil and other anaerobes (e.g., Bacteroides and anaerobic streptococci). These environmental bacteria may enter the muscle through a wound and subsequently proliferate in necrotic tissue and secrete powerful toxins. These toxins destroy nearby tissue, generating gas at the same time. A gas composition of 5.9% hydrogen, 3.4% carbon dioxide, 74.5% nitrogen, and 16.1% oxygen was reported in one clinical case.
Gas gangrene can cause necrosis, gas production, and sepsis. Progression to toxemia and shock is often very rapid.